- Plant Based Estrogen Drugs
- Does Plant Based Estrogen Cause Cancer
- Plant Based Estrogen Replacement Therapy
What are bioidentical hormones?
- PhytoEstrogens (Plant Estrogens) The highest concentrations of Isoflavones are found in soy bean and soy bean products followed by legumes, whereas lignans are the primary source of phytoestrogen found in nuts and oilseeds (e.g. Flax) and also found in cereals, legumes, fruits and vegetables.
- Bioidentical Hormones. Estradiol/Fem Patch-Synthetic.*. Use PhytoEstrogens Not Estrogens A Phytoestrogen is a naturally-occurring plant nutrient that exerts an.
A plant-based estrogen cream may offer some relief from the vaginal dryness and hot flashes women experience. Examples include many of the estrogen patches. Minivelle (estradiol transdermal system) estrogen patches offer relief from hot flashes and night sweats. Bioidentical hormones are defined as man-made hormones that are very similar to the hormones produced by the human body. Common hormones that are matched are estrogen, progesterone and testosterone. These are then used as treatment for men and women whose own hormones are low or out of balance.
Hormones are special chemicals made by parts of the body called glands. They are messengers that tell other parts of the body how and when to work. Hormones control almost all tasks in the body. These include sex and brain function, growth and the breakdown of food. When hormones are out of balance, symptoms can occur.
Bioidentical hormones are defined as man-made hormones that are very similar to the hormones produced by the human body. Common hormones that are matched are estrogen, progesterone and testosterone. These are then used as treatment for men and women whose own hormones are low or out of balance. Some prescription forms of bioidentical hormones are pre-made by a drug company. Other forms are custom-made by a pharmacist based on a doctor’s order. This is called compounding. The US Food and Drug Administration (FDA) has approved a number of preparations of bioidentical estradiol and progesterone, which are molecularly identical to the structure of the hormones generated by the human body. They have been through testing for safety and purity and to be sure each dose has the same amount of hormones. The compounded forms have not been tested and approved by the FDA. Though it is often advertised that products that are made from plants like soybeans and yams are “natural” choices, they are altered greatly in a lab so are no longer natural when done with processing. Both the FDA-approved and compounded hormones come in a variety of doses and routes of delivery (pills, creams, gels, sprays, and vaginal inserts).
Customized bioidentical hormones are often advertised as being a safer, more effective, natural, and an individualized alternative to conventional hormone therapy. However, these claims remain unsupported by any large-scale, well designed studies. Also, the lack of FDA oversight for compounded hormones generates additional risks regarding the purity and safety of custom compounded bioidentical hormones. Although custom hormone combinations often include blends of the same ingredients found in FDA-approved bioidentical hormones (i.e., plant-derived 17β-estradiol or micronized progesterone), some custom compounded preparations include additional hormone varieties (i.e., estriol, pregnenolone, and DHEA). These additional hormones have not undergone adequate testing and are therefore not included in any FDA-approved products.
Why are bioidentical hormones used?
As men and women age, the levels of some key hormones in the body go down. These include estrogen, progesterone and testosterone. This can lead to certain symptoms. Some are very common to women who are past the age of having periods (menopause). Some common effects of low hormones include:
- Hot flashes
- Night sweats
- Loss of energy
- Fatigue
- Loss of muscle mass
- Weight gain
- Foggy thinking
- Mood changes
The treatment is to replace the hormones that have been lost with the hormone therapy. As a result, hormone levels will increase and symptoms will improve. Currently, national societies and expert recommendations state that the risks and benefits of conventional and bioidentical hormones should be considered equal. Your doctor can discuss with you the variety of options available, and guide therapy based on your preferences.
How common are bioidentical hormones?
The use of the compounded type is very common in the U.S. in women in menopause. The North American Menopause Society (NAMS) reports that about 1.4 million women are using this treatment. NAMS notes that that is 40% of all prescriptions for hormone therapy in women who are in menopause. The number of men using this treatment is not noted.
How are bioidentical hormones given?
There are many ways to get bioidentical hormones. These include pills, patches, creams, gels, shots and implanted pellets. Your doctor will decide which method is best for you. You may try more than one way before you find one that works well for you.
How does my doctor select my dose?
People on hormone treatment are watched very closely by their doctors. Most often, doses are adjusted according to a patient’s symptoms and needs, with the goal of keeping the dose to the minimum required to achieve your goals. Depending on your doctor, you might have routine blood, urine or saliva tests to check your hormone levels. Your doctor may adjust your dose based on your changing hormone needs. It should be noted that the FDA recommends against using hormone levels to guide the dosing of hormone therapy in women, as normal levels fluctuate day to day, and vary between patients. In particular, salivary hormone levels are known to fluctuate widely, and have not been shown to be related to menopausal symptoms.
Are bioidentical hormones safe?
The bioidentical hormones that have been approved by the FDA have been tested for safety. They have passed the FDA’s very strict standards and have been shown to be safe for people to use. The compounded hormones have not gone through the FDA’s testing. As yet, little research has been done on them. They have not been proven to be safe or unsafe. Many major medical groups do not support using them because not enough is known about their safety and long-term side effects.
Are compounded bioidentical hormones bad?
There are risks to taking the compounded hormones. But in some cases, they might be the better choice. They might be needed to get the right source (gel, cream, pill, etc.), dose or mix of hormones for a patient. Also, a patient might have a bad reaction to the pre-made form. Your doctor will know which type is better for you.
What are the risks of bioidentical hormones?
It has been shown in research studies that there are risks for women who take hormones, called hormone therapy (HT). It can increase the risk of blood clots, stroke, and gallbladder disease. In women who are older, and who use hormone therapy for an extended period, the risk of heart disease and breast cancer may also increase. Many doctors who use bioidentical hormones claim they are safer than regular HRT. But there have been no large research studies of bioidentical hormones. It has not been shown that they really reduce the risk of these problems.
What are the side effects of bioidentical hormones?
When the FDA approves a drug, the drug company must report on any side effects they are told about, including prominently noting it in the paperwork when picked up at the pharmacy. Pharmacies that compound hormones do not have to report drug side effects to the FDA, or provide such paperwork. This contributes to the myth that compounded hormones are safer, when in fact doctors don’t know all of the possible side effects of these hormones.
Side effects can occur when a dose is first given. The body is not used to the new level of hormones. The dose may need to be changed. Some side effects can be linked to a certain hormone in the mixture. Many side effects get better as the body adjusts to the new level of hormones. Some common side effects include:
- Weight gain
- Tiredness
- Increased facial hair (women)
- Spotting
- Cramping
- Mood swings
You may itch or get red around the area where you get a shot or where you apply your hormones if you use a patch, cream or gel.
When should I call my healthcare provider?
Call your healthcare provider if you have a bad side effect after getting a dose of hormones. If you have a side effect that you cannot manage or does not go away in a short time, your hormone level might be too high.
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Related Institutes & Services
Ob/Gyn & Women's Health Institute
Find the latest information on Women’s Health, including the use of minimally invasive surgical techniques, treatments for infertility, menstrual disorders, urogynecology and pelvic floor disorders, menopause and more.
Glickman Urological & Kidney Institute
The Glickman Urological & Kidney Institute offers innovative treatments in urology and nephrology, including minimally invasive, scarless options for urologic procedures and medical management of kidney disease.
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
NEW YORK (Reuters Health) - A new study adds to evidence that skin patches offer a safer alternative to pills for women who want to treat their menopausal symptoms with hormones.
The study, of 54,000 women who used hormone replacement therapy (HRT), found that those who used estrogen patches were one-third less likely to develop blood clots in the legs or lungs.
That was in comparison to women who used estrogen-only pills. Past studies have found that hormone-patch users have a lower blood clot risk than women who take oral HRT containing both estrogen and progesterone.
But more importantly, the current study gives a snapshot of what’s going on in the “real world,” according to lead researcher Patrick Lefebvre, of Analysis Group, Inc. in Montreal, Canada.
Most of what’s been known about the blood clot risks of estrogen patches has come from clinical trials, Lefebvre told Reuters Health in an email.
The current findings are based instead on health insurance claims from just over 54,000 women who used HRT at some point between 2002 and 2009.
“Our study corroborates the literature with data from the real-world setting,” Lefebvre said.
Analysis Group, Inc. conducted the study with funding from Novartis Pharmaceuticals, a maker of hormone therapy patches.
The number of women using HRT plummeted in 2002 after a large U.S. clinical trial found that women on estrogen-plus-progesterone pills had higher risks of blood clots, heart attack, stroke and breast cancer than placebo users did.
Up to that point, HRT had been prescribed to prevent heart disease and osteoporosis — which experts now advise against.
However, hormone therapy remains the most effective way to ease menopausal hot flashes, so some women with severe symptoms opt for it. Because of the risks, they are advised to use HRT at the lowest dose and for the shortest time possible.
There is growing evidence, though, that low-dose patches may not carry all the risks that pills do.
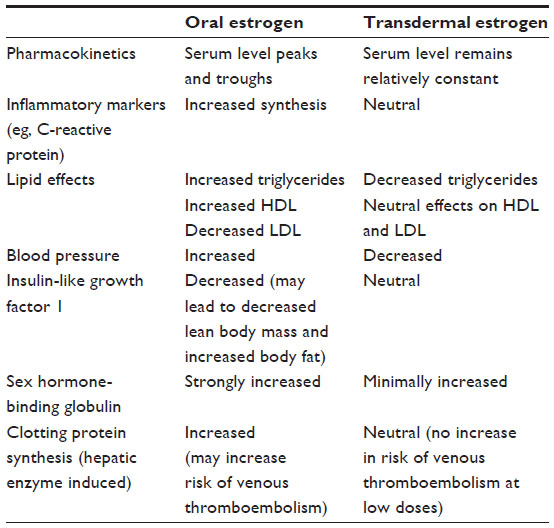
Researchers think hormone patches may be less risky than pills because of the way they work. Unlike oral hormones, those delivered via skin patch bypass the liver, and may not boost clot-promoting proteins in the blood.
In the current study, women used hormone therapy for just over a year, on average.
Plant Based Estrogen Drugs
Of the roughly 27,000 women who used estrogen-only pills, 164 developed blood clots in the leg veins or the lungs — for a rate of almost 0.6 percent per year. Of the 27,000 women who used estrogen patches, 115 developed a blood clot — a rate of 0.4 percent each year.
Blood clots in the lungs are potentially fatal. Clots in the legs are dangerous as well, because they can break off and travel to the lungs, or to arteries supplying the heart or brain, where they can trigger a heart attack or stroke.
Coupled with past studies, the new findings suggest that for women who want to try hormones to ease hot flashes, patches could be a safer alternative.
However, the patches tend to be more expensive than the pills, which usually cost less than $15 a month for generic versions.
But Lefebvre said the bottom line for women is to be aware that there are different options for managing menopausal symptoms. “The decision on how to treat must be an individual one based on discussion with your doctor.”
Some women may be able to ease hot flashes with simple changes, like sleeping in a cool room and watching their intake of caffeine, alcohol and hot, spicy foods. And there’s some evidence that yoga, meditation or other relaxation techniques can be helpful.
Does Plant Based Estrogen Cause Cancer
In some cases of more-bothersome hot flashes, doctors prescribe low doses of certain antidepressants. Vaginal dryness, another common menopause symptom, may be treatable with topical estrogen, which delivers much less of the hormone into the bloodstream versus pills.
As for alternative remedies for hot flashes, some studies have suggested that soy, black cohosh and other sources of phytoestrogens (plant-based estrogen-like chemicals) may help; other studies, however, have found no such benefit.
SOURCE: bit.ly/qBcWd1 Menopause, online July 27, 2011.
Plant Based Estrogen Replacement Therapy
Our Standards:The Thomson Reuters Trust Principles.
